Understanding the Science of Plasma Donation
The Role of Plasma in the Human Body
Plasma is a vital component of blood, constituting about 55% of its total volume. It is a yellowish liquid that serves multifaceted functions, facilitating the transportation of nutrients, hormones, and proteins throughout the body. Composed of approximately 90% water, plasma also contains crucial electrolytes, enzymes, clotting factors, and waste products, making it integral to homeostasis. One of its predominant roles includes maintaining blood pressure and volume, acting as a reservoir that the body can draw upon in times of need. Additionally, plasma is essential for immune function as it contains antibodies that protect against infections. This intricate balance and the dynamic nature of plasma underscore the importance of ongoing research and advances in plasma donation, ultimately highlighting why donations are pivotal in treating patients battling severe medical conditions.
How Plasma Donation Works: A Step-By-Step Journey
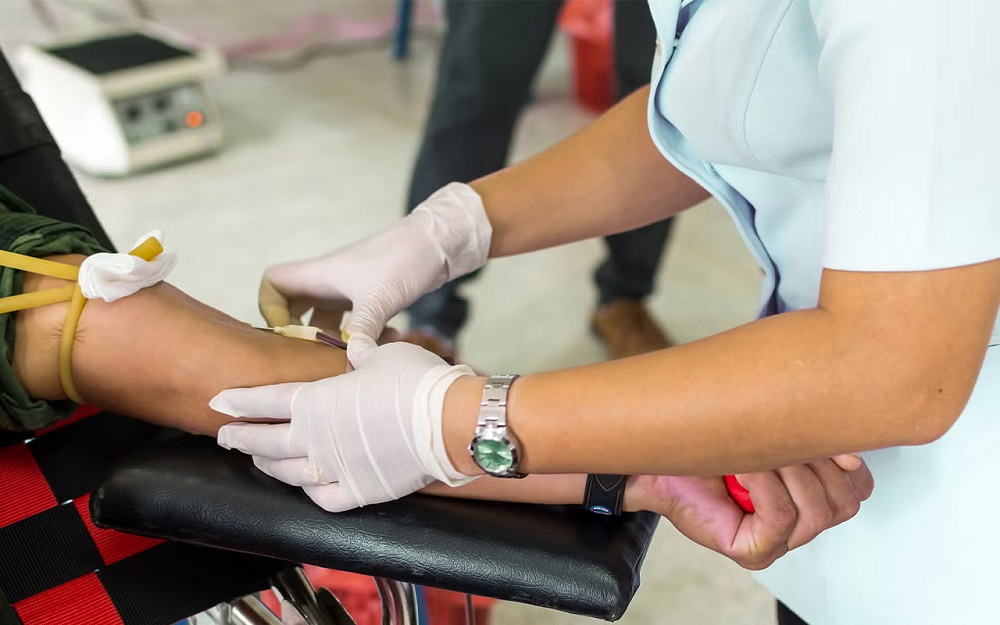
The plasma donation process is both systematic and straightforward, ensuring donor safety and comfort while maximizing the value of each donation. Initially, potential donors are greeted at a donation center, where they undergo basic assessments, including a health questionnaire and a brief medical history review. Following this screening, a phlebotomist checks vital signs and performs a short physical examination to confirm eligibility. Once cleared, donors typically recline in a comfortable chair, and a sterile needle is inserted into a vein, usually in the arm. Unlike traditional blood donation, where whole blood is collected, plasma donation utilizes a process called plasmapheresis. In plasmapheresis, blood is drawn from the body, separated into its components red cells, white cells, platelets, and plasma using a centrifuge, and only the plasma is collected. The remaining blood components are then returned to the donor’s bloodstream. This entire process generally lasts about 60-90 minutes, allowing donors to contribute a significant amount of plasma without jeopardizing their health.
Common Misconceptions About Plasma Donation
Despite increasing awareness around plasma donation, numerous misconceptions continue to persist. A prevalent myth is that donating plasma is painful and dangerous. In reality, while some discomfort is expected during the process similar to having blood drawn there are stringent safety protocols in place that minimize risks. Moreover, many believe that donating plasma is synonymous with losing a substantial amount of blood; however, the procedure only extracts about 600–800 ml of plasma, which is quickly replenished by the body. There is also a misunderstanding regarding eligibility, particularly when it comes to the qualifications to donate plasma; individuals often assume they are disqualified due to minor health concerns. In truth, many medical conditions do not prevent someone from donating, as long as their overall health meets the required criteria. Additionally, some people mistakenly think that plasma donation only benefits the donor; however, it plays a vital role in treating patients with serious medical conditions, highlighting the meaningful impact of contributing to the community.
Who Can Become a Plasma Donor? Unraveling Eligibility Requirements
Age, Weight, and Health Standards: What to Consider
To donate plasma, individuals must meet predefined eligibility criteria that ensure the safety and efficacy of the donation process. Primarily, the donor must be at least 18 years old and weigh a minimum of 110 pounds (50 kg). These regulations are established to safeguard both the donors and recipients; younger individuals and those below the minimum weight threshold may not possess the physiological maturity or body mass necessary for such a donation. Additionally, candidates must demonstrate reasonable health and display no signs of severe illness. Many donor centers require a health screening to assess vital health markers, including blood pressure and hemoglobin levels. It’s also essential that donors maintain a balanced diet, rich in iron and stay hydrated before their appointment to uphold physical well-being throughout the donation. Understanding these guidelines not only prepares individuals for the donation experience but also emphasizes the importance of overall health and well-being in contributing to this life-saving process.
Medications and Medical Conditions: Are You Still Eligible?
Many prospective donors often harbor uncertainties regarding their eligibility based on existing medications or medical conditions. While some medications may preclude individuals from donating plasma, many common prescriptions do not affect eligibility. For instance, certain antibiotics and controlled substances have waiting periods post-consumption before one can donate, primarily for safety reasons. Conversely, individuals suffering from chronic conditions such as asthma or diabetes may still qualify, provided the conditions are well-managed and do not interfere with the donation process. Blood donation centers typically provide comprehensive guidance regarding specific medications and health concerns during the screening process, allowing for individualized assessments. This nuanced understanding of health conditions and their implications for plasma donation reflects the evolving nature of medical guidelines, stressing the importance of dialogue between potential donors and healthcare professionals.
The Importance of a Comprehensive Health Screening
A comprehensive health screening serves as a linchpin in the plasma donation process, ensuring that both the donor and recipient are protected from potential health risks. This screening includes thorough assessments of medical history, lifestyle choices, and any medications currently being taken. During this phase, the donor’s vital signs, such as blood pressure, pulse, and temperature, are meticulously monitored, and blood samples might be taken to assess hemoglobin levels and screen for infectious diseases. The purpose of these assessments is not only to ascertain donor eligibility but also to maintain the integrity of the blood supply and safeguard recipient health. Potential donors are encouraged to address any concerns they may have during this screening, thereby fostering open communication that ensures mutual safety. Such rigorous protocols demonstrate the healthcare community’s commitment to protecting all parties involved while promoting the invaluable act of plasma donation.
The Plasma Donation Process: What to Expect
Preparing for Your First Donation: Tips and Tricks
Preparatory steps before your first plasma donation can enhance the experience and promote successful outcomes. Prior to your appointment, it’s crucial to stay well-hydrated; drinking plenty of water over the days leading up to the donation can improve your plasma volume and help reduce discomfort during the withdrawal process. Eating a nutritious meal rich in protein and iron, such as lean meats, legumes, and leafy greens, will support overall health and increase your hemoglobin levels, which may be evaluated before donation. Furthermore, it is advisable to dress comfortably and wear layers, as the temperature in donation centers can vary. Finally, getting plenty of sleep the night before ensures that you arrive at the center relaxed and ready to donate. These simple yet effective tips can make a considerable difference in the donation experience, not just for the donor but also for the staff and recipients relying on those donations.
The Donation Procedure: From Start to Finish
The donation procedure is streamlined to create a comfortable and efficient environment for donors. Upon arriving at the center, donors check in and complete any necessary paperwork. A healthcare professional will then take you through the preliminary health assessments mentioned earlier. Once cleared, you will be guided to a donation chair, where a sterile needle will be inserted into your arm. Following the setup, the process of plasmapheresis begins. A specialized machine separates the blood components, collecting plasma while returning red blood cells and platelets to your body. It is vital to remain relaxed during this process, as tension can impede blood flow. For those who may experience anxiety, it is helpful to engage in distractions such as listening to music or bringing a book or other forms of entertainment. Once the process is complete, the healthcare staff will remove the needle, apply pressure to the site, and bandage it. The overall procedure typically lasts around 60-90 minutes, during which donors play a crucial role in saving lives.
Post-Donation Care: Staying Healthy After Donating
After donating plasma, it’s essential to dedicate some time to post-donation care to foster quick recovery and sustain overall well-being. Most donation centers require a brief recovery period that typically involves resting for at least 10 to 15 minutes. During this time, donors are encouraged to consume snacks and rehydrate, as replenishing lost fluids and nutrients aids in recovery. It is advisable to avoid strenuous activities for the remainder of the day, allowing the body to recuperate and recover fully. Many donation centers recommend keeping the bandage on for several hours to prevent any bleeding. Additionally, any feelings of dizziness or fatigue should be reported immediately, as healthcare professionals are trained to assist in these situations. By adhering to these guidelines, donors can ensure their well-being while preparing their bodies for future donation opportunities.
Debunking Myths: The Truth Behind Plasma Donation Risks
Are There Real Risks Involved? Evaluating Safety Factors
While fears about risks associated with plasma donation are prevalent, understanding the actual safety measures can help mitigate these concerns. Plasma donation is regarded as a generally safe procedure when carried out professionally at licensed facilities. Health risks associated with donation primarily include minor complications such as bruising, soreness, or adverse reactions to the needle. Serious risks, such as infection or severe allergic reaction, are exceedingly rare due to stringent safety protocols, including the use of sterile equipment and comprehensive screening of donors. Furthermore, donors undergo education regarding potential side effects, thus empowering them to participate with confidence. The plasma collection centers have thorough protocols for managing any complications that might arise, ensuring immediate care is available. This context not only alleviates concerns but affirms the dedication of healthcare professionals to donor safety in the noble act of saving lives.
The Impact of Repeated Donations on Your Health
Understanding the long-term implications of repeated plasma donations is critical for both potential and current donors. The human body has a remarkable capability to regenerate plasma, typically replenishing the donated plasma volume within 24-48 hours. However, many centers recommend that individuals donate no more frequently than once every 28 days to allow full recovery of plasma protein levels and overall health. Research indicates that while most individuals tolerate frequent donations well, consistent monitoring and a balanced diet are necessary to maintain health. Adverse effects of over-donation could potentially include low protein levels and dehydration if donors do not properly care for themselves. By adhering to recommended timeframes for donations and being mindful of hydration and nutrition, donors can contribute significantly to life-saving treatments while safeguarding their health in the long run.
Real Stories: Donors Share Their Experiences
Nothing encapsulates the spirit of plasma donation quite like the authentic stories of those who have participated in this life-changing process. Many donors describe profound feelings of fulfillment and connection knowing that their contributions directly impact patients in need. For instance, a cancer survivor may share how receiving plasma products during treatment saved their life, motivating them to give back by becoming a donor themselves. Other donors emphasize the community aspect of donor events and the friendships forged in waiting rooms and donation chairs, reinforcing a sense of camaraderie among those dedicated to helping others. Such firsthand accounts serve as powerful testimonials, inspiring others to consider the potential to save lives through plasma donation. By sharing these stories, donors not only uplift their narratives but also foster awareness and education about the importance of plasma donation.
Overall, this extensive guide provides a detailed overview of the crucial qualifications, processes, myths, and realities surrounding plasma donation, aimed at educating and encouraging potential donors on their journey to making a significant and life-enhancing impact in the healthcare community. By delving deeply into the science, eligibility requirements, and shared experiences, readers can leave not only informed but also inspired to consider becoming plasma donors themselves.